A Step-by-Step Guide on the Procedure for Dental Implants
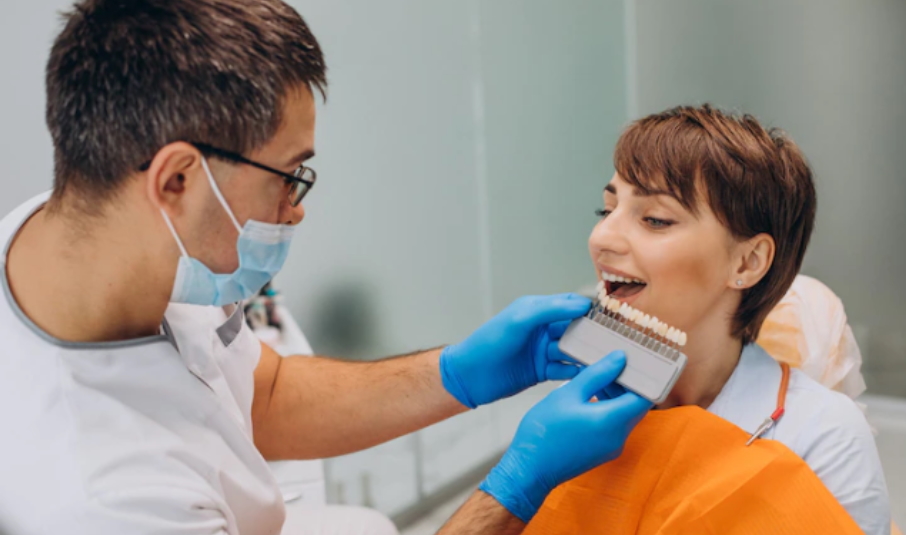
A dental implant is a surgical procedure whereby a metal post is placed into the jawbone to serve as a replacement for a missing tooth. The post is then capped with a dental prosthetic, such as a tooth, bridge or denture, to restore the smile.
Dental implants are a popular choice for those who have lost a tooth or teeth due to injury, disease or decay. The implants are strong and durable, and they can last a lifetime with proper care. Dental implants can be an expensive investment, but they are often worth the cost because of the many benefits they offer. Implants can improve the look of your smile and boost your self-confidence. They can also make it easier to eat and speak.
If you are considering dental implants, it is important to know the step-by-step guide for the procedure of dental implants. This will help you to understand what to expect and to be prepared for each step of the process. Here is a step-by-step guide to the dental implant procedure:
- The first step is to have a consultation with your dentist to see if you are a good candidate for dental implants.
Dental implants are a terrific way to restore your smile and replace missing teeth. Dental implants are not appropriate for everyone, though. Consultation with your dentist to determine your suitability for dental implants is the first step. Your dentist will check your teeth and gums during the consultation to make sure they are in good enough shape to sustain the implants. Additionally, X-rays will be taken to assess the condition of your jawbone. If dental implants are right for you, your dentist will create a treatment plan just for you.
- Next, your dentist will place the implants into your jawbone.
After your initial consultation and exam, your dentist will determine whether dental implants are the right solution for you. If they are, the next step is to place the implants into your jawbone. This is a minor surgical procedure that is usually performed under local anesthesia. Your dentist will make small incisions in your gums and then place the implants into your jawbone. Once the implants are in place, your dentist will close the incisions with stitches.
- Once the implants are in place, you will need to wait for them to heal and integrate with your jawbone.
Once the implants are in place, you will need to wait for them to heal and integrate with your jawbone. This can take several months, and during this time you will need to be careful with your oral hygiene and avoid putting too much pressure on the implants.
- Once the implants are healed, you will return to your dentist to have the artificial teeth (called crowns)
Once your implants have healed, you will need to return to your dentist to have the artificial teeth (called crowns) placed on them. This is necessary to ensure that your implants are properly taken care of and to ensure that you have the best possible results. This will complete the dental implant process and give you a beautiful, natural-looking smile.