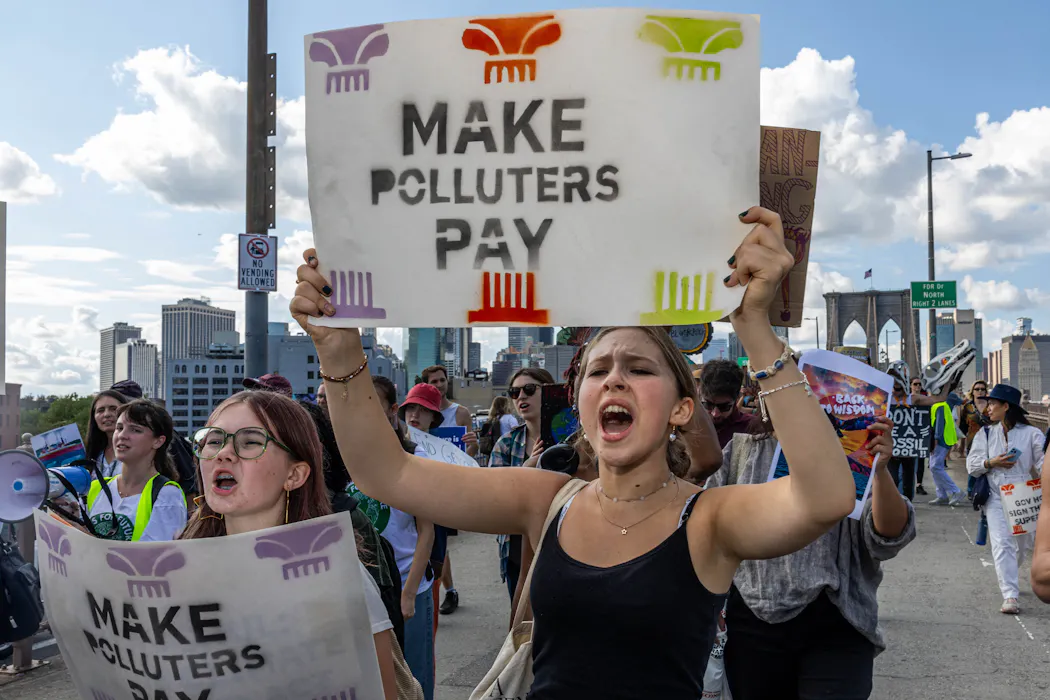Real-life decisions: why price signals for Medicare are flawed
 Responses to small price signals may be more emotional than rational, but they're real. AAP Image/Dave Hunt
Responses to small price signals may be more emotional than rational, but they're real. AAP Image/Dave HuntAmid last week’s furore over the on-again, off-again Medicare co-payment proposal, Prime Minister Tony Abbott emphasised during Question Time that his government wanted “to see price signals in the system” in relation to public health and Medicare.
The principle of price signals is a compelling one – it forces people to weigh the benefits they receive against the costs of the resources they are using. This helps prevent wasteful use of our national resources, which is what economic efficiency is all about.
That said, there is a fundamental flaw: in an essential health system such as Medicare, flat-charge price signals have the capacity to hurt most those who are least able to afford its services.
A recent survey assessed 47 international studies on the behavioural effects of co-payments for health care. It found low-income people in poor health reduced their use of health services proportionally more than others.
Australian daily life is littered with instances of seemingly minor imposts exerting a far greater influence on behaviour than anyone could possibly have imagined. Why would health care be any different?
The classic example in the lives of commuters is toll-avoidance. Melbourne and Sydney are full of rat-running and toll avoidance every day of the week. The average price of a single toll trip might be only A$3.30 but this affects lived behaviour profoundly. It does not necessarily force people out of cars into public transport, to car-pool, or to telecommute. But it does mean that intersections at either end of a toll road are jammed at peak hour.
Take another example: petrol dockets. For a discount of just four cents per litre, thousands of motorists will clip coupons and will drive out of their way to branded petrol stations that honour their discount vouchers. Is this rational? Based on an average tank capacity of 60 litres, the total saving is less than A$2.50. Many drivers spend much of that “discount” just driving to the station.
 Some motorists go to extraordinary lengths to avoid tolls.TK Kurikawa/Shutterstock
Some motorists go to extraordinary lengths to avoid tolls.TK Kurikawa/Shutterstock
So powerful was this “small price signal” that in February 2014 the Australian Competition and Consumer Commission took formal action against the two major supermarkets for apparently not adhering to a promise to limit their fuel docket values, since they were skewing buyer behaviour so dramatically. Since the co-branding regime began, the market shares of Coles Express and Woolworths Caltex have risen to claim over 48% of the petrol-purchasing public. Many independent operations have simply closed.
This may be more emotional behaviour than a rational response. But it is real, nonetheless.
And the list goes on: Many people get intensely upset over A$2.00 charges for baggage trolleys at the airport. They are irked when their mobile phones drop out in a transmission dead-zone and they have to ring a number again. The average cost of a re-dial? Less than 29 cents.
Toll evasion on public transport is a serious, ongoing issue. The average cost of a journey? Less than A$3.00.
Many businesses add 1% (or more) of the purchase cost solely because the customer is paying with a credit card. Another major grumble.
Many pensioners will ask businesses to please provide them with a landline number to ring, because the former is about 40% cheaper than a call to a mobile number. The average saving per phone call? Less than 20 cents.
In the real world, small and personal price signals really do matter. So the argument that a A$7 fee hike for GP visits will not affect behaviour in negative ways doesn’t hold.
As many medical peak bodies have already observed, the one certainty is that the most vulnerable members of the community will be the most adversely affected. Even more: that patients with less serious ailments will flood emergency departments of public hospitals instead – those same waiting rooms that are already filled to overflowing.
Levying a A$7 co-payment for everyone who fronts up at the doctor’s office — regardless of their means — is just asking for trouble. Order a blood test for cholesterol? Another A$7. Get an x-ray to make sure your back injury is muscular and not skeletal in nature? Ditto.
 Co-payments disproportionately affect low-income groups.Grenville Turner/AAP Image
Co-payments disproportionately affect low-income groups.Grenville Turner/AAP Image
Discouraging people from seeing their GP is counter to all sensible trends in preventative medicine. For the past 30 years, every cogent public health campaign has emphasised the importance of early diagnosis (of skin and breast cancers, of asthma, of diabetes).
This is especially true in the case of Indigenous health campaigns. The uphill battle has been one of persuading First Nations people to trust and visit their GPs in the first place. Over the past six months, Aboriginal medical services across the country have slammed the co-payment idea for just that reason and have vowed not to charge it.
The biggest health insurers — including the recently privatised Medibank Private — have proven the worth of the preventative approach. Over the past decade, managing director George Savvides has overseen clever initiatives such as the adding of points to any Medibank subscriber’s Flybuys account if they buy fresh or frozen fruit and vegetables from Coles supermarkets.
Can anyone doubt the importance of small price-signalling there? Or the premise that a milligram of prevention is worth a kilogram of cure? This is being undermined by an inflexible Medicare co-payment proposition that refuses to die.
Finally, the stated motivation for the co-payment — which is to help repair the budget and contain health spending — has been undermined by splurging A$5 of the co-payment on a medical research fund. This is not to deny the importance of medical research — far from it. But why ask the poor and sick to bear a disproportionate burden of the cost?
This has to be looked at seriously. It has to be looked at now. The price-signalling evidence suggests that the Medicare co-payment proposal should be buried once and for all on the floor of the House of Representatives.
The authors do not work for, consult to, own shares in or receive funding from any company or organisation that would benefit from this article. They also have no relevant affiliations.
Read more http://theconversation.com/real-life-decisions-why-price-signals-for-medicare-are-flawed-34851