Rotavirus cases in children are rising – but a highly effective vaccine has slashed hospitalizations from the virus by 80% in 2 decades
- Written by Annette Regan, Adjunct Associate Professor of Epidemiology, University of California, Los Angeles
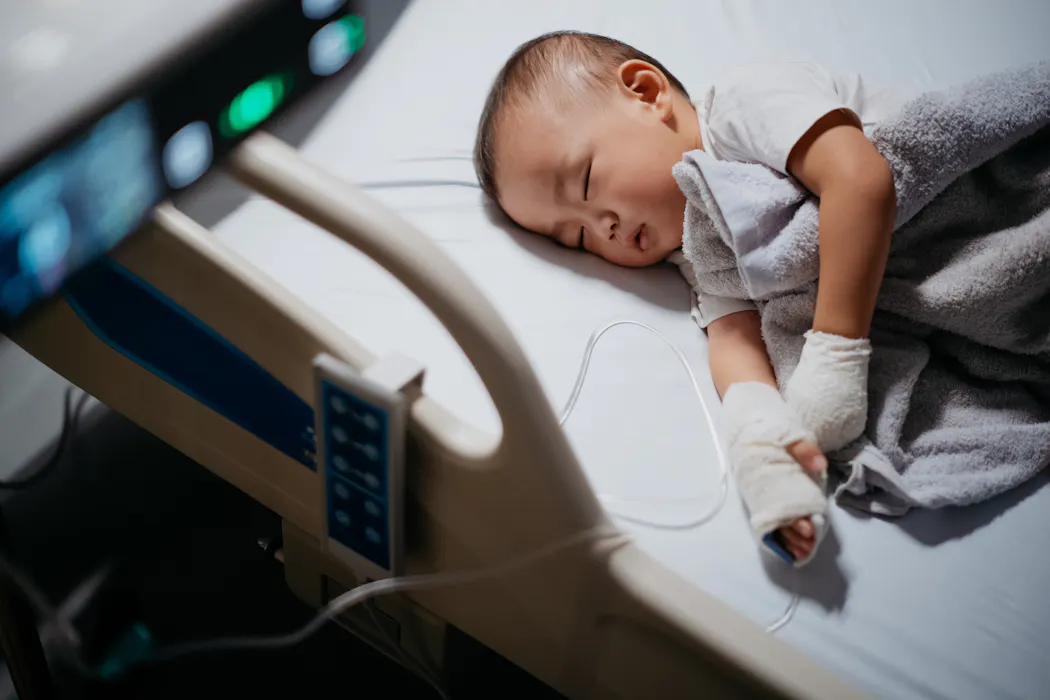 One of rotavirus infection's main symptoms is diarrhea, which can lead to severe dehydration that needs to be treated in the hospital.hxyume/E+ via Getty Images
One of rotavirus infection's main symptoms is diarrhea, which can lead to severe dehydration that needs to be treated in the hospital.hxyume/E+ via Getty ImagesRotavirus is a highly contagious virus that spreads easily and can make babies and young children very sick. This year, doctors have been seeing more cases earlier in the season than usual.
Data from the Centers for Disease Control and Prevention shows that almost 8 in 100 people tested for rotavirus have the virus. This is only a little higher than last year at this time, when about 7 in 100 tests were positive. However, doctors are concerned because rotavirus cases started rising earlier than usual – in January – which means more children are getting sick over a longer period of time.
Often referred to as a stomach flu or stomach bug, rotavirus infection can cause extreme diarrhea, leading to severe dehydration and hospitalization. Just like measles and whooping cough, infectious diseases that are also on the rise, rotavirus can be prevented with a safe and highly effective vaccine. But vaccination rates in the U.S. have fallen since 2018.
The Conversation asked epidemiologist Annette Regan to explain why this virus is on the rise and what families can do to protect themselves from the illness.
What is rotavirus and why is it dangerous?
Rotavirus, first identified in 1973, affects the gastrointestinal system – that is, the stomach and the intestines.
Rotavirus spreads from person to person, often when germs from poop get on hands or surfaces and then into the mouth. But a person can also become infected by touching a contaminated surface and then touching their mouth, or by drinking or eating contaminated food or water.
Rotavirus causes sudden diarrhea, vomiting and fever that can cause rapid dehydration, which can lead to death if left untreated. There is no medicine to cure the virus. Doctors can only help by giving fluids and watching closely for dehydration. Babies who lose too much fluid may need care in the hospital.
Rotavirus most often affects infants and young children. Without vaccination, nearly all children have a rotavirus infection by age 5.
The virus causes most instances of hospitalization due to severe diarrhea and is the leading cause of death due to diarrhea in children under 5. Older children and adults typically experience more mild infections, but the virus can cause severe illness in people with weakened immune systems and those over 65.
A safe and effective vaccine
Safe and effective vaccines against rotavirus have been available in the U.S. since 2006.
U.S. regulators approved an early rotavirus vaccine, but it was taken off the market the next year after doctors learned that, in very rare cases, it could cause a serious bowel problem. The rotavirus vaccines used today are different. Studies in more than 70,000 babies show that these vaccines are safe and work well.
Before vaccines were introduced, rotavirus accounted for more than 400,000 medical visits, including 200,000 emergency room visits, 70,000 hospitalizations and 20-60 deaths in the U.S. each year.
Annually, vaccination prevents an estimated 40,000-50,000 hospitalizations of infants in America. Since 2006, hospitalizations due to rotavirus have dropped by 80% and emergency room visits by 57%.
Acute diarrhea caused by viral illness can be lethal for babies and young children.Recent rotavirus surge
Rotavirus is a springtime illness in America. Cases usually increase over the winter and reach their highest point around April or May, then drop off as the weather gets warmer in the summer.
Since January 2026, doctors have been seeing more rotavirus in babies and young children than usual. According to CDC data, about 3% of rotavirus tests in January were positive, when normally only about 1% of tests are positive. That rate is now peaking at nearly 8% of tests.
Scientists have also found more rotavirus by monitoring community sewage to track how germs are spreading. The levels of virus in sewage have gone up by about 40% since February. Together, this tells doctors that rotavirus is spreading more widely and lasting longer than it usually does, which is why they are watching it closely.
Rotavirus vaccine rates in the U.S. have been declining – 77% of children received the full vaccine series by 8 months of age in 2018 compared to 74% of children in 2024. That leaves more infants susceptible to infection. Rotavirus surges are generally shorter in areas where more people are vaccinated against it, meaning they could last longer in areas with lower vaccination coverage.
In January 2026, the Department of Health and Human Services shifted rotavirus vaccination from a universal recommendation to a decision to be made by families and their health care providers. Although this change was recently paused by a U.S. judge, this has left public health officials increasingly concerned that rotavirus vaccination rates could continue to decline.
Preventing rotavirus infection
Proper hand-washing can help reduce rotavirus transmission, but because rotavirus is highly contagious, preventing the disease through vaccination is the most effective form of protection.
There are two oral, live‑attenuated rotavirus vaccines available for infants in the U.S. The first dose must be given before 15 weeks of age, and all doses must be completed by 8 months of age.
Rotavirus vaccines reduce the risk of severe disease in infants by 85% to 90%. This means fewer hospital visits, less risk of dehydration and more babies staying healthy at home.
But these benefits last only when most babies get vaccinated. When vaccination rates drop, rotavirus can spread more easily, and more infants, especially the youngest ones, can get seriously ill. Keeping vaccination rates high helps protect individual babies and keeps the whole community safer.
Annette Regan receives research and related funding from the National Institutes of Health, Pfizer Inc, Moderna, and Merck Sharp & Dohme paid to her institution. She consults for the Pan American Health Organization and is affiliated with Kaiser Permanente Southern California.
Authors: Annette Regan, Adjunct Associate Professor of Epidemiology, University of California, Los Angeles